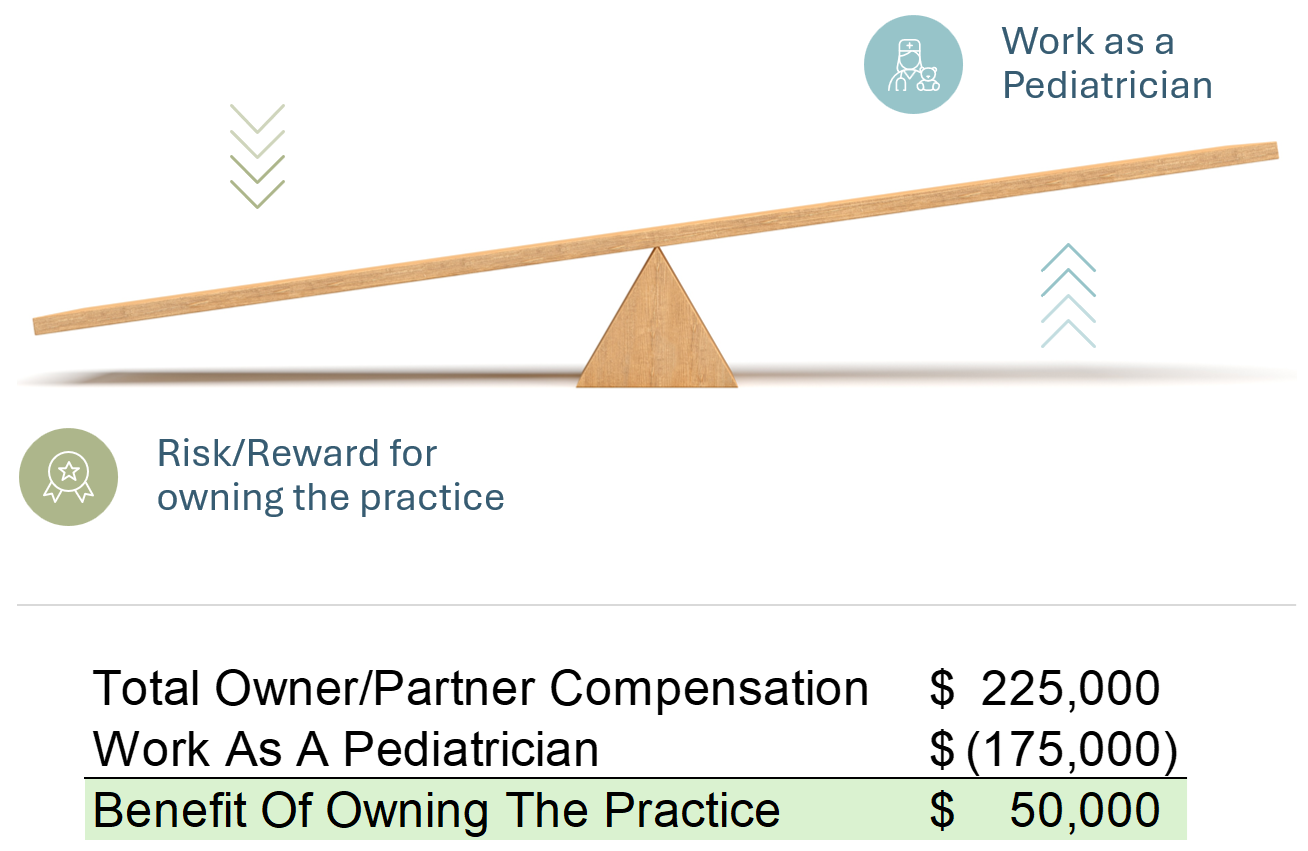
Not All Revenue Is Created Equal
Ask most pediatric practice owners how they get paid and the answer usually starts with something like "we split everything evenly" or "it all goes into one pool." That explanation is understandable — simplicity has real value in a busy practice. But it often masks a more complicated reality: the ten or more revenue streams flowing into a typical pediatric practice do not all work the same way, and treating them as if they do can quietly undermine physician satisfaction, distort incentives, and create friction between partners.
This article walks through why revenue streams differ, how each one flows through your expense structure, and how those flows ultimately translate into distinct components of owner compensation. If you have ever wondered why two physicians with similar productivity end up with materially different earnings — or why compensation discussions seem to generate so much heat — the answer often lives in these distinctions.
A pediatric practice is not one business. It is several businesses operating under the same roof — each with its own economics, its own cost drivers, and its own implications for who gets paid what.
The Grocery Store Problem
A modern grocery store runs produce, a bakery, packaged dry goods, a deli counter, and often a pharmacy — all under one roof, all contributing to one revenue line. But no rational grocer would evaluate the produce section using the same metrics as canned goods, or allocate costs the same way across a fresh bakery and a packaged cereal aisle. The spoilage risk, the labor intensity, the margin profile, and the customer behavior are fundamentally different.
Pediatric practices face exactly the same challenge. Well-child visits, vaccine drugs, laboratory services, behavioral health, telemedicine, capitation arrangements, quality incentive programs, revenue generated by employed physicians, and revenue generated by employed extenders all land on the same revenue line — but they carry entirely different cost structures, reimbursement patterns, and connections to individual physician effort. Allocating all of them through a single pool ignores those differences entirely.
The consequence is not just theoretical. When a high-volume vaccine practice splits vaccine margins evenly, the physician whose patient panel generates 35% of vaccine revenue receives the same vaccine earnings as the physician generating 10%. Over time, such a misalignment, and others, accumulate into compensation dissatisfaction, partner disputes, and potential departures that could have been avoided.
The Twelve Revenue Streams — and Why They Are Not Interchangeable
Before getting to allocation methods, it helps to be specific about what the revenue streams actually are. A typical independent pediatric practice draws revenue from 12 common streams, each with its own economics and appropriate allocation approach.

Five Allocation Approaches — and When Each Applies
PMI recommends that practices adopt a deliberate mix of expense allocation strategies rather than defaulting to a single method for all revenue. Below are the five approaches most commonly used in well-designed pediatric compensation plans.
Direct Allocation — Assign to the owner
Costs assigned specifically to the individual who generated them. A physician's salary, benefits, CME, personally performed hospital services — when attribution is clear, direct allocation is the most equitable method.
Even Split — Equal for all partners
Practice-wide revenues and costs that benefit all partners equally — rent, accounting, shared infrastructure, and revenue generated by employed physicians and extenders. Simple and defensible, but breaks down when applied to streams with meaningful variation across providers.
Productivity-Based (wRVU) — More visits, more cost
Higher patient volume drives higher resource consumption. Medical supply consumption scales with the number of patients seen. wRVU-based allocation distributes these proportionally to the physicians driving the activity.
Vaccine-Based — Vaccine volume share
Vaccine drug margins are typically allocated based on each physician's proportionate share of total vaccine revenue generated. If a physician accounts for 20% of vaccine revenue, they should, in theory, receive 20% of the vaccine drug margin — far more equitable than an even split. However, depending on the practice's culture, the practice may elect to share some of the vaccine profits evenly across all partners simply because the practice is managing the inventory and juggling the available cash to ensure the vaccine invoices are paid.
Hybrid — Fixed + variable blend, often 50/50
Not every cost falls cleanly into one bucket. Some expenses have a dual nature — part fixed, part performance-driven — which is where hybrid cost models come in. Hospital practice support coverage, capitation, and quality incentives are good examples: they carry a shared component alongside a variable layer tied to individual provider contribution(s). Certain staffing costs work the same way.
Consider a practice that determines it needs at least three people at the front desk to keep the flow of patients into the office running smoothly. That number is fixed regardless of what's happening on any given day. But if that practice has three providers and one of them is responsible for half of all patient visits, it stands to reason that provider is consuming a disproportionate share of the front office's time and resources. Treating that cost as purely fixed glosses over a real operational reality.
That's precisely the scenario where a hybrid allocation model can start to make a lot of sense.
Click here to access PMI's Interactive Revenue Flow — From Source to Owner Earnings
How Revenue Flows Into Owner Earnings
Once revenue is allocated through the appropriate method, it flows into distinct components of owner compensation. Making these components explicit serves both transparency and trust — physicians who understand which streams contribute what to their earnings can have compensation conversations grounded in operational reality rather than generalized grievances about fairness.

The distinction between these buckets matters not just for compensation design but for how physicians understand and discuss their earnings. A physician who sees high volume but manages a Medicaid-heavy panel may have modest vaccine earnings and strong production incentives. A physician who leads the behavioral health program may have lower base salary but meaningful behavioral health provider earnings. Partners whose practices employ physicians and extenders will see margin from those relationships flow into a dedicated Employed Provider Earnings bucket rather than the general pool. Surfacing all of these components explicitly allows for compensation conversations grounded in operational reality.
At a glance — Revenue stream, allocation method, and owner earnings bucket
|
Revenue stream |
Allocation method |
Owner earnings bucket |
|
Well visits |
wRVU + Even split |
Base salary + Production incentives |
|
Sick visits |
wRVU + Even split |
Base salary + Production incentives |
|
Vaccine drugs |
Vaccine-based |
Vaccine earnings |
|
Vaccine administration |
wRVU |
Base salary |
|
Lab services |
Hybrid |
Lab earnings |
|
Hospital — personally performed |
Direct allocation |
Base salary |
|
Hospital — practice support |
Hybrid |
Practice hospital support |
|
Behavioral health |
Direct allocation |
Behavioral health earnings |
|
Telemedicine |
wRVU + Even split |
Base salary |
|
Capitation |
Hybrid |
Capitation / PMPM |
|
Quality incentives |
Hybrid |
Quality incentives |
|
Employed physicians |
Even split |
Employed provider earnings |
|
Employed extenders |
Even split |
Employed provider earnings |
Aligning Incentives With Practice Strategy
The allocation framework is not just a compensation tool. It is a strategy tool. The choices a practice makes about how to allocate revenue send clear signals about what the partnership values — signals that every physician on staff reads, whether or not the topic is ever discussed explicitly.

A practice that allocates vaccine margin through an even split signals that immunization performance is a collective effort. A practice that allocates vaccine margin based on individual vaccine revenue share signals the opposite — and will likely see physicians paying more attention to their own immunization rates as a result.
Similarly, a practice that creates a dedicated behavioral health earnings bucket sends a clear signal that it values behavioral health integration and wants to compensate the physicians investing in it. A practice that lumps behavioral health revenue into the general pool sends the opposite signal, regardless of what the strategic plan says.
|
|
|
|
|
|
Where to Start
If your practice currently uses a single-pool compensation model, moving to a multi-stream allocation framework does not have to happen all at once. PMI typically recommends a phased approach: begin by mapping which revenue streams your practice actually has, then identify which two or three allocation distinctions would have the greatest impact on physician satisfaction and incentive alignment. Implement those first, measure the results, and expand from there.
The goal is not complexity for its own sake. A compensation plan that no one understands is not a good compensation plan regardless of how mathematically precise it is. The goal is a system that is transparent enough for physicians to understand their earnings, honest enough to reflect operational reality, and fair enough that the partnership can sustain it through disagreements and transitions.
The goal is not to make compensation more complicated. It is to make it more honest — so that physicians understand what they are earning, why they are earning it, and what levers they can pull to influence it.
Getting there requires a clear-eyed look at how your revenue actually flows — from the source, through the allocation method, and into the owner earnings buckets that determine what each physician takes home. That is a conversation PMI is glad to help you start.
|
Ready to rethink how your practice allocates revenue? PMI specializes in helping independent pediatric practices design compensation systems that align financial outcomes with practice values. Reach out to discuss your situation with one of our consultants. Schedule a Conversation > pediatricsupport.com/practice-assessment |